
Although depression is an extremely common mental disorder, impacting over 17 million people just in the United States, effective medical options for treating depression remain limited. While psychotherapy can be effective in some cases, there are many people who need additional treatment.
Current antidepressant medications are more or less a trial-and-error process, each with its own varying side effects. Over 60% of patients do not experience relief from the first antidepressant they try, and each following medication is less likely to be effective. Many people find this process overwhelming and exhausting, and may or may not end up finding relief with a medication that they then must rely on for the foreseeable future.
Now there are two promising options for those struggling with treatment-resistant depression: TMS and ketamine therapy. Let’s take a look at both.
What is TMS?
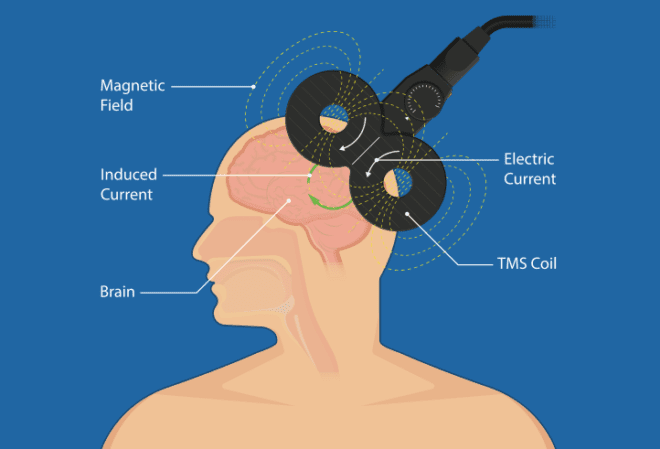 TMS means transcranial magnetic stimulation. This refers to the process of using magnetic pulses to activate specified neural areas in the brain. TMS therapy for treating depression involves targeting areas in the brain that are under-active and known to be associated with depression, in order to stimulate neural activity and boost neuroplasticity.
TMS means transcranial magnetic stimulation. This refers to the process of using magnetic pulses to activate specified neural areas in the brain. TMS therapy for treating depression involves targeting areas in the brain that are under-active and known to be associated with depression, in order to stimulate neural activity and boost neuroplasticity.
TMS treatment is an extremely safe, non-invasive process, with minimal risks and side effects. Transcranial magnetic stimulation has been used in clinical trials since 1985 to measure neural activity. The most common type of TMS therapy is Express TMS, which only takes a few minutes to administer by applying the TMS device onto the scalp. A standard treatment plan consists of 5 TMS sessions per week for six weeks. Typically patients report a light tapping sensation on the scalp during treatment.
The most commonly reported side effects include a mild headache or lightheadedness that usually subsides shortly after the treatment is over. TMS may not be approved for treating depression in individuals prone to seizures or with metal implants.
The most impressive part is the results: over 60% of patients see significant symptom relief and 40% experienced complete remission. Not only that, but once treatment is over, most people continue to have symptom relief for six months to a year or longer. This is one of the only forms of treating depression that shows prolonged effectiveness; most antidepressants stop working as soon as you stop taking them.
What is Ketamine Therapy?
 Ketamine treatment involves administering specified doses of ketamine via an IV or a nasal spray a few times a week for 2-3 weeks. In higher doses, ketamine has been used medically as an anesthetic since the 1950’s. At lower doses, it offers minimal risks, few side effects, and is clinically proven to have antidepressant effects. Over half of patients experience symptom relief within 5 hours after their first dose, and a large percentage have relief for many months after the treatment period has ended.
Ketamine treatment involves administering specified doses of ketamine via an IV or a nasal spray a few times a week for 2-3 weeks. In higher doses, ketamine has been used medically as an anesthetic since the 1950’s. At lower doses, it offers minimal risks, few side effects, and is clinically proven to have antidepressant effects. Over half of patients experience symptom relief within 5 hours after their first dose, and a large percentage have relief for many months after the treatment period has ended.
A typical treatment period consists of 6 sessions spread over the course of 2-3 weeks. Booster sessions can be scheduled as needed to extend the effectiveness of the treatment.
There are two types of ketamine treatment: ketamine infusion and esketamine nasal spray. The infusions are administered intravenously by a medical physician. The nasal spray contains esketamine or S-ketamine, a slightly different type of ketamine sold as Spravato, and can be self-administered under medical supervision.
The most commonly reported side effects of treating depression with ketamine are dizziness or a floating sensation, mild hallucinations, and feeling tired after treatment. Patients are required to have someone drive them home from treatment sessions but then may continue their normal routine.
Depression treatment clinics like Bespoke Treatment offer both TMS and ketamine therapy in a comfortable environment by licensed physicians. Additionally, depending on your medical history and the medications you’ve tried in the past, you can get both of these options covered by your insurance company.




Be the first to comment